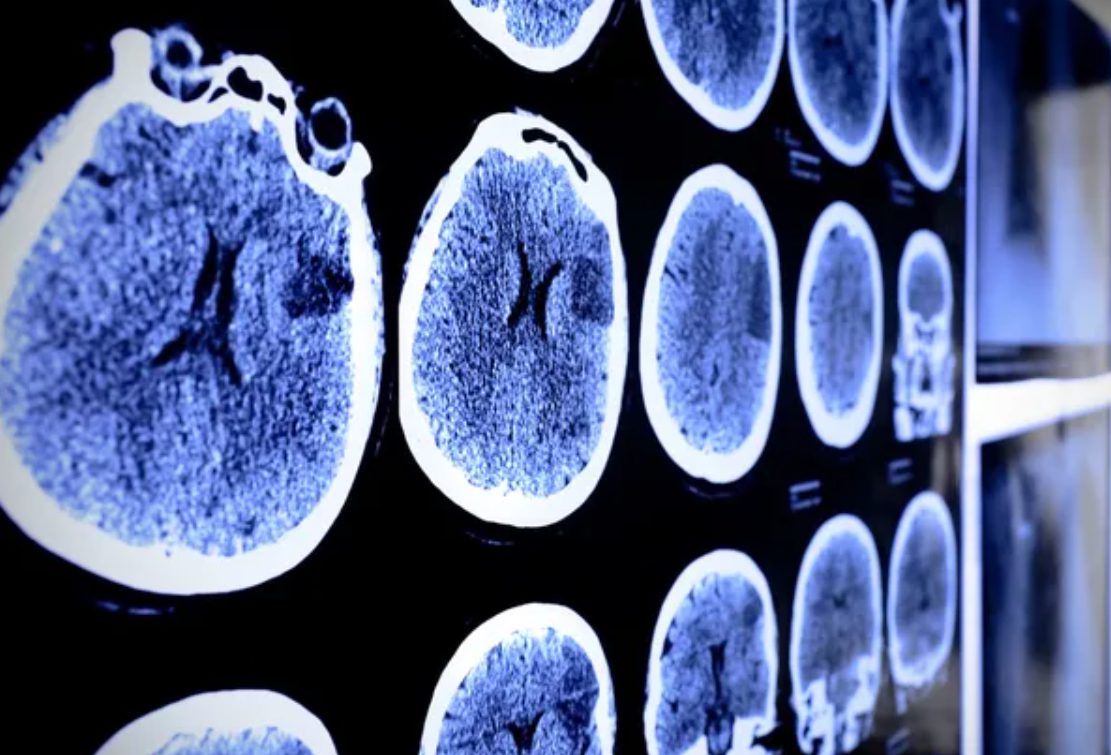
Stroke damage was considered permanent until Swiss and American scientists proved otherwise. In a September study published in Nature Communications, University of Zurich and USC researchers transplanted human neural stem cells into stroke-damaged mouse brains—and watched paralyzed animals regain movement as new neurons literally rebuilt their motor circuits.
The results sound like science fiction, but they’re documented with AI-powered gait analysis that tracked each mouse’s recovery over weeks. Unlike previous stem cell attempts that merely reduced inflammation, these neural progenitor cells (derived from induced pluripotent stem cells) survived five weeks after transplantation, matured into functional neurons, and integrated into existing brain networks through specific signaling pathways.
Beyond Band-Aids: Actual Brain Reconstruction
The transplanted cells triggered multiple repair processes simultaneously, from growing new blood vessels to strengthening protective barriers.
“Our findings show that neural stem cells not only form new neurons, but also induce other regeneration processes,” explains Christian Tackenberg from the University of Zurich. Think of it like renovating a house after flood damage—you’re not just patching walls, you’re rebuilding the electrical system, plumbing, and foundation simultaneously.
The cells promoted:
- Blood vessel growth
- Reduced harmful inflammation
- Strengthened blood-brain barrier that protects neural tissue
Previous studies using different cell types showed promise through indirect effects, but this marks the first demonstration of direct tissue replacement restoring lost function. When your brain loses neurons to stroke, getting them back changes everything.
Reality Check: The Long Road to Human Trials
Despite promising results, patients face years of testing before these treatments reach clinical practice.
Before you start planning your recovery around stem cell therapy, remember that mouse brains aren’t human brains. The researchers still need to validate safety concerns including immune rejection and long-term integration in larger animal models.
Human trials could begin within the next few years, but FDA approval typically requires another decade of testing. Still, this represents genuine progress for the 15 million people worldwide who suffer strokes annually. The treatment window—one week post-stroke rather than hours—could fundamentally expand recovery options.
For families living with stroke’s aftermath, that timeline shift alone justifies cautious optimism about reversing damage once considered irreversible.